What you need to know about prostate cancer
Did you know 1 in 5 males are at risk of developing prostate cancer by age 85, making it the most common internal cancer in Australian men? In fact, more men die of prostate cancer each year than women do of breast cancer, with an estimated 3,500 deaths in 2018.
This is a sobering statistic and is only set to rise, increasing from 2,711 deaths in 2001 to 3,102 in 2014 and expected to reach 25,000 in 2020. This means men need to be more aware of their risk now more than ever. So here’s what you need to know about prostate cancer.
What is prostate cancer?
According to the Prostate Cancer Foundation of Australia, prostate cancer occurs when abnormal cells develop in the prostate (a walnut-sized gland in the male reproductive system located below the bladder and in front of the rectum). These abnormal cells can continue to multiply in an uncontrolled way and sometimes spread outside the prostate into nearby or distant parts of the body.
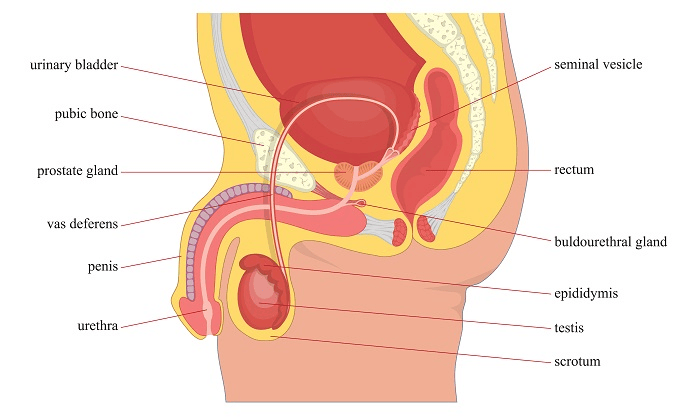
There are three different stages of prostate cancer:
1. Localised prostate cancer – When the cancer is only found in the prostate gland.
2. Locally advanced prostate cancer – When the cancer has extended beyond the prostate and may include seminal vesicles or other surrounding organs such as the bladder or rectum.
3. Metastatic prostate cancer – When the cancer has spread to distant parts of the body such as the bone.
What are the symptoms?
Generally a slow growing disease, the majority of men with low grade prostate cancer can live for many years without symptoms and without it spreading and becoming life-threatening. However, high grade disease spreads quickly and can be lethal, therefore appropriate management is key.
So while in the early stages there may be no symptoms, in the later stages some of the symptoms might include:
- Feeling the frequent, urgent or sudden need to urinate
- Finding it difficult to urinate
- Discomfort or pain when urinating
- Weaker than normal stream
- Flow that stops and starts
- Feeling like you haven’t completely emptied your bladder
- Finding blood in urine or semen
- Painful ejaculation
- Erectile dysfunction
- Pain in the lower back, upper thighs, hips, pelvis or chest
- Weak or numb legs and feet
- Tiredness, shortness of breath, dizziness, fast heartbeat or pale skin
If you experience any of these symptoms, you should go and see your doctor (especially if you find blood when you urinate).
What are the risk factors?
Risk factors to consider:
- Age: Prostate cancer is an age-dependent disease, which means the chance of developing it increases rapidly from age 50.
- Family history: If you have a first degree male relative with prostate cancer, you have a higher chance of developing it than men with no such history. This risk increases again if more than one male relative has prostate cancer or if those male relatives were diagnosed when young.
- Genetics: Changes in certain genes that can be carried in families such as mutations in the BCRA1 or BCRA2 genes may increase the risk of developing prostate cancer in some men. People with a genetic condition called Lynch syndrome also have a higher risk.
- Diet & lifestyle: There is some evidence to suggest that eating a lot of processed meat or food that is high in fat can increase the risk of developing prostate cancer. Your environment and lifestyle may also play a part.
Some other risk factors to also be aware of include:
- Having a family history of breast or ovarian cancer
- High testosterone levels
- Males of African descent are at higher risk
How is it detected and diagnosed?
For many men prostate cancer is often curable if detected early, particularly if the disease is confined to the prostate gland. It is therefore important that men who have any of the risk factors mentioned above have regular checkups with their GPs.
A number of tests may be performed to investigate symptoms of prostate cancer and confirm a diagnosis, but the two most common are a blood test or physical examination:
1. PSA – A blood test to check for prostate-specific antigen (a protein produced by the prostate) as the level of PSA can be higher than normal in people with prostate cancer.
2. DRE – A digital rectal examination where the doctor inserts a gloved finger into your rectum to feel the prostate through the rectal wall.
If either of these tests confirm a patient may be at risk of prostate cancer, the doctor will then arrange a biopsy. A biopsy is when a urologist removes small samples of tissue from the prostate, which is then sent off to test if the cells are cancerous or non-cancerous. A biopsy is the only way to confirm a diagnosis of prostate cancer.
How to reduce the risk
It is very difficult to prevent a prostate cancer diagnosis, but there are many lifestyle choices men can make to lower their risk and keep the prostate health. Some of these include:
- Exercising regularly
- Reducing intake of fats (including red meat and dairy products)
- Eating more fish (high in omega-3 fatty acids and other ‘good fats’)
- Eating plenty of fruits and vegetables (increases intake of antioxidants)
- Avoiding smoking
- Only drinking alcohol in moderation
- Making a conscious effort to reduce stress in both work and home life
Was this helpful? Contact us now if you need more information about prostate cancer or to make an appointment for a prostate check.
